What’s Really Holding Back Tech in Physical Therapy
Written by: Brianna Hodge
If you’ve ever paused before trying a new piece of technology in your clinic, I want you to hear this clearly: You’re not behind. You’re thoughtful.
In physical therapy, that matters more than being early. Because every decision you make touches someone’s recovery, someone learning to walk again, someone managing pain, and someone trying to return to a version of life they recognize.
So when people ask why more clinics haven’t adopted new technology, the answer isn’t that clinicians are resistant, it’s that clinicians are responsible. You’re weighing outcomes, safety, time, and trust, all at once.
But something is shifting right now. Technology in rehabilitation, especially virtual reality and artificial intelligence, is no longer experimental. It’s becoming usable, measurable, and increasingly aligned with how you already practice.
The real question isn’t whether you should adopt it. It’s how to do it in a way that actually works for you, your patients, and your day-to-day reality.
The Gap Between Innovation and Reality
There’s no shortage of innovation in healthcare right now. You’ve likely seen it in conferences, journals, or even on your own social feeds; Virtual reality systems, AI documentation tools, motion tracking platforms, and digital engagement solutions. On paper, they promise better outcomes, stronger engagement, and more efficient workflows.
And to be fair, many of those promises are supported by research. Studies on virtual reality rehabilitation show improvements in motor function, patient motivation, and adherence across neurological and musculoskeletal populations (Tang et al.). AI tools are increasingly capable of reducing documentation burden and identifying meaningful clinical patterns.
But if you step back and look at most clinics today, many are still operating in familiar ways. Traditional exercises, manual documentation workflows, and limited use of immersive or data-driven tools still dominate.
This disconnect isn’t because clinicians don’t care about innovation. It’s because availability does not equal adoption. Healthcare research consistently shows that even when technology is accessible, adoption depends on far more complex factors; workflow fit, trust, training, and organizational readiness (G).
What Actually Holds Clinics Back
Time Is Already Spoken For
You don’t have unused space in your day. You’re managing back-to-back sessions, documenting in between, adjusting interventions in real time, and constantly thinking about patient safety and progress.
When new technology enters that environment, it isn’t competing with curiosity, it’s competing with time. If something slows you down, even slightly, it’s hard to justify continuing to use it. Research consistently highlights workflow disruption as one of the biggest barriers to adoption, and you’ve likely felt that firsthand.
Past Experiences Shape Present Decisions
Most clinicians have tried something before that didn’t quite deliver. Maybe it looked impressive during a demo but didn’t translate well clinically. Maybe it required too many steps, or maybe patients simply didn’t engage with it the way you expected.
Those experiences matter. They shape how you evaluate new tools moving forward. Studies on AI adoption emphasize that trust and perceived usefulness are critical, if a system doesn’t clearly improve patient care, it won’t be used, no matter how advanced it is (Ahmed et al.).
Training Feels Like an Investment Without a Guarantee
Learning something new always comes with a cost. Not just in time, but in energy. And the question that naturally follows is whether that investment will actually pay off.
Healthcare technology research repeatedly shows that lack of training and ongoing support leads to failed implementation. It’s not that clinicians aren’t capable of learning new systems, it’s that the return on that learning has to be clear and immediate.
Cost Is Bigger Than a Price Tag
When clinics evaluate new technology, they’re not just thinking about upfront costs. They’re considering how it affects operations. Will it take up space? Will it require additional staff time? Does it align with reimbursement? Will it actually improve outcomes enough to justify the shift?
These are practical questions, and they’re valid ones.
Culture Shapes Adoption More Than Features
Even the best technology will struggle in an environment that isn’t ready for it. If a clinic is already stretched thin, or if leadership isn’t aligned, or if workflows are inconsistent, introducing something new becomes exponentially harder.
Research across healthcare systems shows that organizational readiness often determines success more than the technology itself (Greenhalgh et al.). In other words, adoption isn’t just about the tool, it’s about the environment it enters.
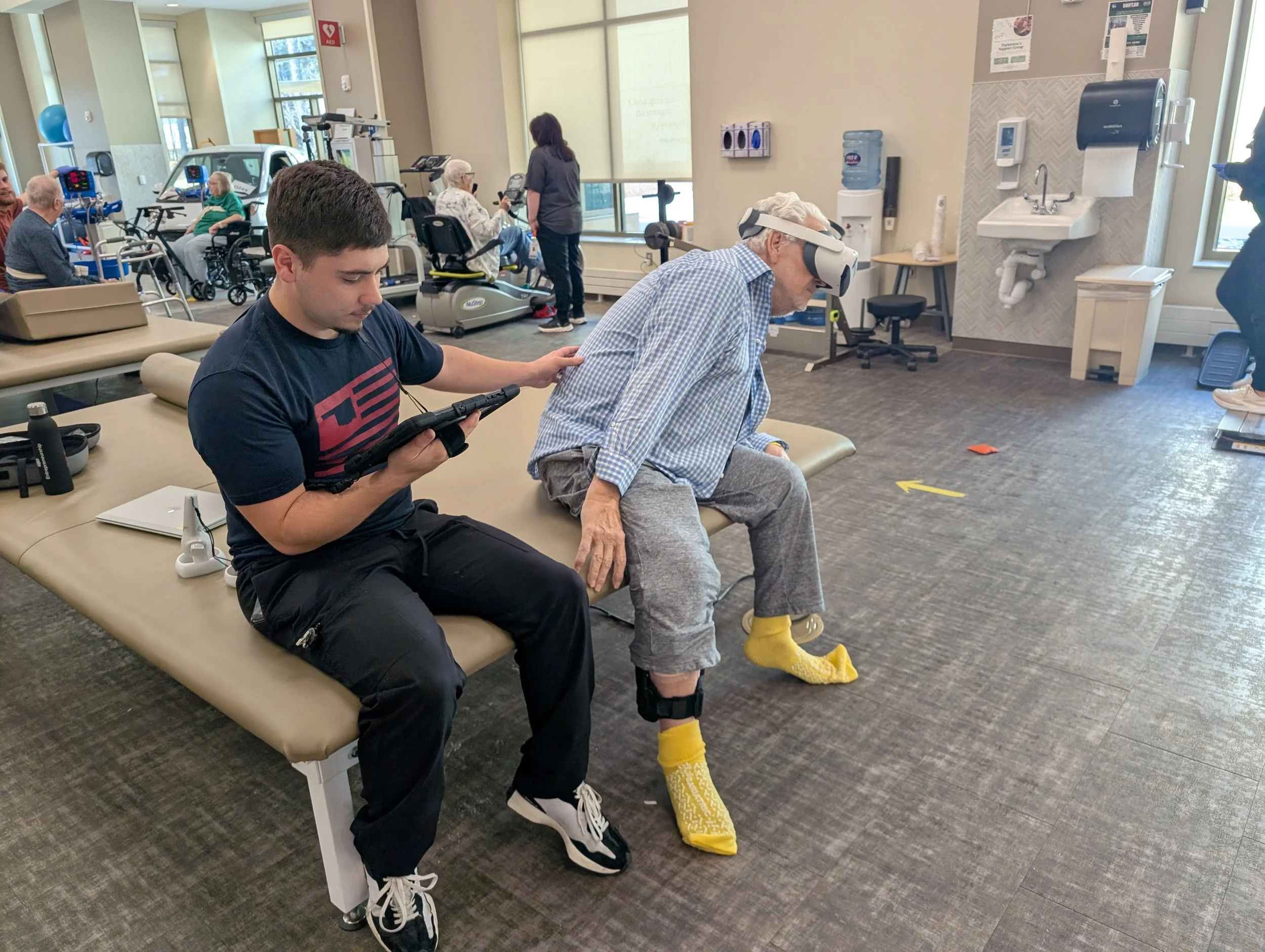
Virtual Reality in Physical Therapy: What It Really Looks Like
Virtual reality has become one of the most talked-about technologies in rehabilitation, but what matters isn’t the concept, it’s how it shows up in practice.
Clinically, VR allows you to place patients in environments that would otherwise be difficult or impossible to recreate. It creates opportunities for repetition without monotony and engagement without forcing it. Instead of asking a patient to complete another set of the same movement, you’re guiding them through an experience that requires those movements naturally.
Research supports this shift. VR has been shown to improve upper extremity recovery after stroke, increase adherence to therapy, and enhance patient satisfaction. In neurodegenerative conditions and musculoskeletal rehabilitation, it has demonstrated measurable improvements in function and motivation (Tu et al.).
But the real impact isn’t just in the data. It’s in the subtle changes you notice during sessions. Patients stay engaged longer, ask to continue, and move more freely because they’re focused on the task, not the effort.
That shift in engagement is not a small detail. It’s often the difference between minimal participation and meaningful progress.
AI in Physical Therapy: The Change You Feel More Than You See
While VR is visible, AI tends to operate quietly in the background. But its impact is just as significant.
In physical therapy, AI is increasingly being used to assist with documentation, analyze patient data, and streamline workflows. Instead of spending large portions of your day writing notes, AI systems can help generate structured documentation based on session data.
This matters because documentation is not just a task, it’s a source of fatigue. Reducing that burden doesn’t just save time; it changes how you experience your workday.
Studies have shown that AI can meaningfully reduce administrative workload, allowing clinicians to spend more time focusing on patient care. But beyond efficiency, there’s something else happening. When cognitive load decreases, clinical presence increases. You’re able to be more attentive, more engaged, and more responsive during sessions.
That’s where AI’s real value shows up, not in replacing clinical thinking, but in supporting it.
Why Adoption Is Finally Starting to Shift
For a long time, the barriers to adoption felt fixed. But they’re starting to change.
Technology is becoming easier to use, with faster setup times and more intuitive interfaces. Training is becoming more practical, often integrated into workflows rather than existing as a separate burden. Outcomes are becoming easier to measure, giving clinics clearer insight into what’s working and why.
Perhaps most importantly, technology is beginning to align more closely with how clinicians already think and work. Instead of requiring a complete shift in practice, it’s starting to integrate into existing approaches.
This alignment is what makes adoption possible.
How to Implement Technology Without Disrupting Your Workflow
The biggest mistake clinics make when introducing new technology is trying to do too much at once. Successful adoption doesn’t come from sweeping changes. It comes from small, intentional steps.
It often starts with a single use case. A specific goal. Maybe improving balance training for a certain group of patients, or increasing engagement in sessions where motivation has been a challenge. From there, it becomes about applying the technology in a focused way, rather than spreading it across every patient immediately.
Integration matters more than replacement. The most effective tools don’t force you to abandon your current approach. They fit into it. They support what you’re already doing and enhance it.
Consistency also plays a larger role than intensity. Using a new tool for a few minutes each session, over time, often creates more impact than trying to overhaul an entire treatment plan at once.
And throughout this process, feedback, especially from patients, becomes one of the most valuable guides. Their engagement, their responses, and their willingness to continue often tell you more than any metric.
What Successful Clinics Do Differently
Clinics that adopt technology successfully aren’t necessarily more advanced or better resourced. What sets them apart is how they approach change.
They don’t rush it. They don’t try to force adoption across the entire team immediately. Instead, they create space for gradual integration. They allow clinicians to build familiarity and confidence over time.
They also focus on impact rather than novelty. The goal isn’t to use technology because it’s new. It’s to use it because it improves something meaningful, whether that’s patient engagement, functional outcomes, or workflow efficiency.
Over time, these small shifts accumulate. What starts as a single use case becomes part of the clinic’s broader approach.
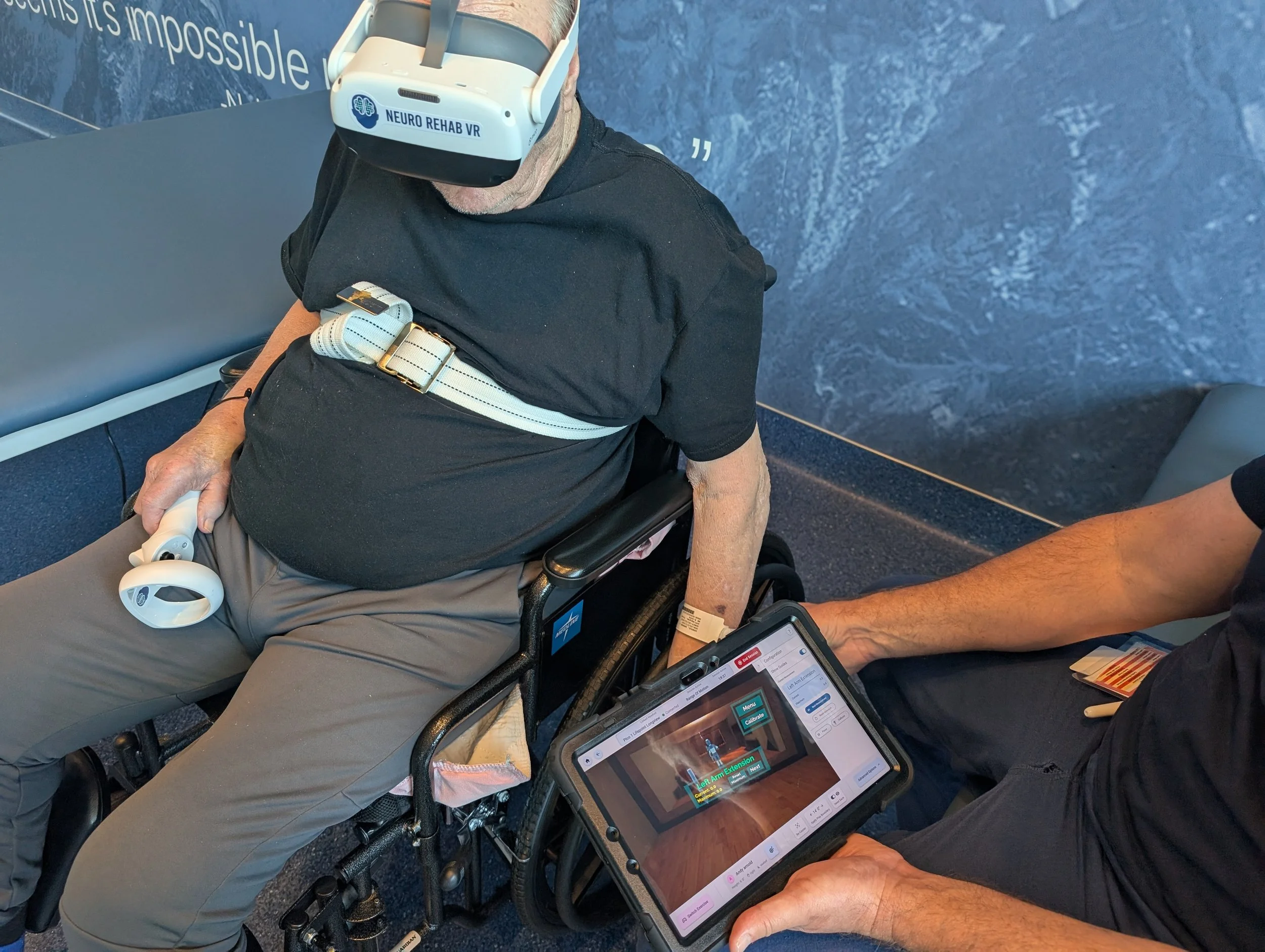
A Real-World Example: Smart Therapy in Practice
When you look at how systems like the Smart Therapy Complete Console are being used in real clinics, you start to see how these ideas come together.
One of the biggest shifts is how naturally it fits into existing sessions. Instead of requiring a full setup or dedicated space, it can be introduced quickly, even within a standard appointment. That alone removes one of the most common barriers.
Clinically, it allows therapists to work on meaningful tasks in a different way. Patients can practice activities that resemble real life, like navigating a grocery store or performing daily routines, while still targeting specific therapeutic goals. For patients who aren’t yet able to stand, it provides opportunities to work on trunk control, coordination, and engagement in a seated position.
At the same time, the system supports clinicians on the operational side. AI-generated documentation reduces time spent on notes, which helps address one of the most persistent sources of burnout in the field.
What makes this kind of technology effective isn’t just what it does, it’s how it fits. It aligns with the pace of clinical work, supports patient engagement, and integrates into workflows without requiring a complete overhaul.
What the Research Consistently Shows
Across multiple studies, the factors that lead to successful adoption are remarkably consistent. Technologies that are easy to use, clearly beneficial, well-supported through training, and aligned with clinical workflows are far more likely to be adopted and sustained.
Patient response also plays a critical role. When patients are more engaged, more motivated, and more willing to participate, clinicians are naturally more inclined to continue using the tool.
These findings reinforce something you likely already know intuitively. Adoption isn’t about convincing clinicians to change. It’s about providing tools that make change feel worthwhile.
The Shift From Resistance to Readiness
There’s a narrative that clinicians are resistant to technology, but that’s not what’s actually happening, instead is discernment.
Clinicians are becoming more selective. More thoughtful about what they bring into their practice. And that selectivity is leading to better outcomes, because it ensures that adoption is driven by value, not novelty. The shift we’re seeing now isn’t from resistance to acceptance. It’s from hesitation to readiness.
Final Thoughts: Change Doesn’t Have to Be Overwhelming
If there’s one thing to take from all of this, it’s that adoption doesn’t have to be all or nothing.
You don’t need to transform your entire clinic overnight. You don’t need to commit to a system before you understand how it fits.
Change can start small, it happens with one patient, one session, and then one moment. Where something feels more engaging, more efficient, or more effective, and from there, it builds.
Because when technology truly supports your clinical thinking, and when it aligns with how you already care for patients, it stops feeling like something new. Instead it starts feeling like something that should have been there all along.
-
Ahmed, Molla Imaduddin, et al. “A Systematic Review of the Barriers to the Implementation of Artificial Intelligence in Healthcare.” Cureus, vol. 15, no. 10, 2023, www.ncbi.nlm.nih.gov/pmc/articles/PMC10623210/.
Apell, Petra, et al. “Explaining the Slow Adoption of AI Innovations in Healthcare: A Network Analysis Approach (Preprint).” JMIR AI, 12 May 2024, https://doi.org/10.2196/60458. Accessed 8 Dec. 2025.
Cresswell, Kathrin, and Aziz Sheikh. “Organizational Issues in the Implementation and Adoption of Health Information Technology Innovations: An Interpretative Review.” International Journal of Medical Informatics, vol. 82, no. 5, May 2013, pp. e73–e86, www.sciencedirect.com/science/article/pii/S1386505612001992, https://doi.org/10.1016/j.ijmedinf.2012.10.007.
Fei, Jiang, et al. “Artificial Intelligence in Healthcare: Past, Present and Future.” Stroke and Vascular Neurology, 21 June 2017, pubmed.ncbi.nlm.nih.gov/29507784/.
G, Vial. “Vial, G. (2019). Understanding Digital Transformation a Review and a Research Agenda. The Journal of Strategic Information Systems, 28, 118-144. - References - Scientific Research Publishing.” Www.scirp.org, 2019, www.scirp.org/reference/referencespapers?referenceid=3502402.
Greenhalgh, Trisha, et al. “Diffusion of Innovations in Service Organizations: Systematic Review and Recommendations.” The Milbank Quarterly, vol. 82, no. 4, Dec. 2004, pp. 581–629, onlinelibrary.wiley.com/doi/full/10.1111/j.0887-378X.2004.00325.x?sid=nlm%3Apubmed, https://doi.org/10.1111/j.0887-378x.2004.00325.x.
Sarka Banikova, et al. “Patient Satisfaction and Tolerance of Virtual Reality Rehabilitation in Subacute Ischemic Stroke: A Pilot Study.” Frontiers in Rehabilitation Sciences, vol. 6, 26 Aug. 2025, https://doi.org/10.3389/fresc.2025.1660766.
Tang, Peiyuan, et al. “The Efficacy of vr in the Application of Musculoskeletal Diseases: An Umbrella Review (Preprint).” Journal of Medical Internet Research, 21 July 2024, https://doi.org/10.2196/64576.
Tu, Tiantaixi, et al. “Benefits of Virtual Reality Rehabilitation on Neurodegenerative Diseases: A Systematic Review.” Npj Digital Medicine, vol. 9, no. 1, 9 Dec. 2025, www.nature.com/articles/s41746-025-02171-3, https://doi.org/10.1038/s41746-025-02171-3.